Surgical treatment of Dupuytren's contracture
- Are you just starting to explore treatment options for your Dupuytren's contracture? Perhaps your GP referred you here? You're in the right place! We can help you get a full explanation of the surgical solution to your Dupuytren's contracture.
Dupuytren's contracture
Dupuytren's contracture is a condition in which the finger(s) of the hand curve inwards. The bending is caused by thickening and shortening of the fibrous tissue in the palmar fascia beneath the skin of the palm, which also affects the position of the fingers. This contracture limits finger motion makes it difficult to carry out everyday activities such as driving, holding hands, playing sports, holding objects.
The disease was first described by Napoleon Bonaparte's doctor, Guillaume Dupuytren, in 1831.

Dr. György Kocsis PhD
Orthopaedic trauma surgeon and hand surgeon, assistant professor, specialist in wrist, elbow and shoulder surgery, upper limb specialist
ONLINE APPOINTMENT BOOKING – BOKOR STREET CLINIC
Please select the appropriate service
The follow-up consultation fee is valid for 3 months after the initial examination, for the same complaint.
- 1. Select the service you need from the drop-down box!
- 2. Use the calendar to choose a date that suits you!
- 3. Enter your details to register or login with your previous registration!
- 4. If you would like to make a reservation on behalf of someone else (e.g. your child), please let us know at the location provided.
- 5. Briefly describe your complaints!
- 6. Select the type of consultation: initial examination, control examination or prescription.
- 7. Click on the button to book your appointment. Thank you for choosing BMM!
If you are unable to make the appointment you have already booked, please, at least 24 hours before notify us of your intention to withdraw. This gives other patients the opportunity to get the medical care they need in time. Thank you for your cooperation and understanding!
Resignation: +36 1 44 33 433
If you cannot find an available appointment for your chosen week, please call our call center on +36 1 44 33 433 for assistance. Our staff will be happy to help you make an appointment with the doctor of your choice or another specialist according to your complaint.
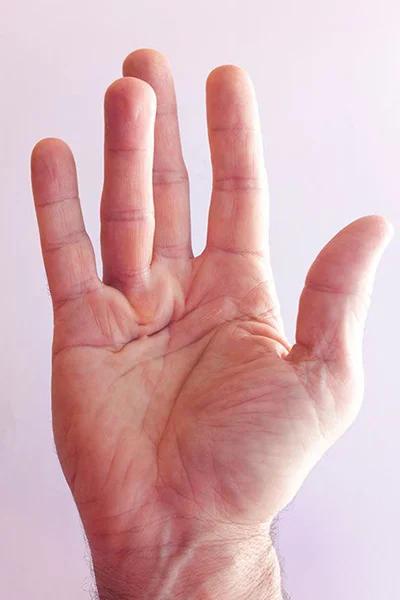
Anatomy of the palm
In the palm of the hand, a layer of connective tissue lies beneath the skin to protect the nerves, blood vessels and tendons that run underneath. A disease of this connective membrane, called Dupuytren's contracture, usually affects the ring and little fingers, but it can also affect other fingers.
Initially, the disease appears as firm nodules develop in the palm, later developing into a hard,cord-like band towards the fingers. As a result, the finger begins to bend into the palm and the patient can no longer fully extend it.
These nodules do not cause any symptoms initially, but may cause tenderness or discomfort when pressed. Later, the extension of the affected fingers is limited. In the final stage, the fingers are locked in a curled constraint.
Causes of Dupuytren's contracture
Dupuytren's contracture is basically a genetic disease, and often runs in families vagy with a strong familial tendency Also:
- It is often associated with diabetes and affects many more men than women.
- It is more prevalent in northern European countries than in southern Europe, which is why some people refer to it as a Viking disease.
- The disease is painless, which is why many people see a doctor at an advanced stage. In such cases, palmar contracture is not only aesthetically disturbing, but the bent fingers can also be disturbing:
- During work
- While driving
- Handshake
- Wearing gloves
- In cleaning
- It often appears on both hands.
Surgical treatment of Dupuytren's contracture is indicated if if cords develop or if the patient is unable to fully extend the finger or fingers. The smaller the loss of movement, the better the outcome after surgery. If the fingers are already in the palm of the hand, the surgical treatment is more difficult, the risk of complications increases andrecovery and rehabilitation may take longer.
The Dupuytren's contracture surgery procedure
The surgeon performs the surgery by making a zig-zag incision from the palm to the finger to open up and release and remove the diseased, thickened palmar fascia. This removal and mobilisation of the joints allows the finger or fingers to be stretched.
We use a tourniquet so that the bleeding from the wound does not interfere with the doctor's work. First, an elastic bandage is wrapped around the affected side forearm to drain blood from the limb vagy empty the veins in the arm. A cuff, similar to a blood pressure cuff, is then placed on the upper arm and pressurised to temporarily stop the circulation to the limb. At the end of the operation, the blood in the wound is drained from the surgical site through a plastic tube.
The surgery is performed under general anaesthesia or axillary anaesthesia, so the patient will not be uncomfortable with the tourniquet cuff on the upper arm, which allows for easier execution and shorter surgery time.
Depending on the extent of the disease, several skin incisions may be used, and the diseased palmar fascia may be partially or completely removed.
The surgery will take into account any previous surgery for similar reasons and any scars that may have resulted.
Eligibility for surgery
Your surgeon will review your medical history and perform a thorough physical examination.
The diagnosis of Dupuytren's contracture is mainly based on physical examination (visual inspection, palpation of the hand and measurement of joint range of motion).
Surgery is recommended if you have so much bending of the fingers that you are already experiencing a significant deterioration in your quality of life that the symptoms prevent it:
- In daily activities
- During work
- While driving
- In sport
- In sport
- Hobby
- Handshake
- When wearing gloves
- In cooking
- In cleaning
Attila Bereczki's recovery story
Our hand specialists

Dr. György Kocsis PhD
Orthopaedic trauma surgeon and hand surgeon, assistant professor, specialist in wrist, elbow and shoulder surgery, upper limb specialist
Preoperative preparation and rehabilitation for Dupuytren's contracture surgery
We all want the surgery to be as successful as possible. The following knowledge is designed to improve the outcome of surgery, reduce the risk of complications and make surgery as safe and effective as possible.
Step 1
Be healthy before surgery!
Blood glucose
You should have a blood glucose test at the planning stage. If you are already diagnosed with diabetes, please check your blood glucose regularly in the weeks before surgery. Well-controlled blood sugar significantly reduces the risk of wound infection. We will also measure your blood glucose levels before surgery and if your blood glucose level is too high, surgery may need to be postponed.
Smoking
If you smoke, please do not smoke in the month before your operation. Smoking impairs microcirculation, which can lead to wound healing problems, so it is important for your own safety that you do not smoke at this time. You will not be able to smoke for at least 24 hours after the operation.
Nutrition
It is very important to eat right: eat plenty of fresh, colourful vegetables and fruit, and get enough protein (meat, eggs, fish). A balanced diet also contributes to wound healing and regeneration. Please also pay attention to your fluid intake and do not start dieting at this time: insufficient food intake will hinder wound healing!
Skin care
Take care of your hands, moisturise them, soften your skin, condition your nails, beware of minor injuries (I'm thinking of scratches from pets)
Plan your surgery: what to do before and after
After hand surgery, your operated hand needs to rest for a few days, so it is important to prepare for the post-operative period.
- Do as much as possible with your unaffected hand in the 1–2 days before surgery.
- Since the wound and dressing cannot be exposed to water after the operation as long as the sutures are in place, try washing in rubber gloves!
- Do the cleaning, shopping and cooking in advance so you don't have to do it with freshly operated hands.
- You should not drive with an operated hand (see Frequently Asked Questions for more information), and we do not recommend public transport because of the potential risk of injury. Please plan your journey home in advance.
- If you have a well-established painkiller, it's a good idea to make sure you have some at home.
Step 2
Getting started -
The last visit before surgery
They will discuss it with the specialist who operated on you:
- The preoperative findings
- Taking medication: paying particular attention to drug sensitivity and taking anticoagulants
- Whether you need an additional nerve ultrasound examination
- If additional testing or consultation with a doctor (e.g. cardiologist) was necessary, this will be discussed again with the surgeon who performed the surgery, and it will be discussed how long any anticoagulant can be taken or whether it is necessary to switch to another medicine
- After a detailed explanation, consent is given, which is a prerequisite for the operation
Step 3
The day of the operation
On the day of your operation, nurses will arrange for you to be accommodated in a ward until the operation, where you can wait comfortably with your companion. Please be sure to remove any jewellery you have brought with you.
Your blood pressure is checked.
Before surgery, please wash your hands and forearms thoroughly with soap.
The surgeon will take you into the operating theatre, lay you on the operating table and place a cuff similar to a blood pressure monitor on your arm, which will keep your arm in place during surgery and minimise bleeding from the wound.
The anaesthetist doctor and his assistant administer anaesthesia, or an axillary anaesthesia, known as a guided anaesthetic.
Step 4
Going home
After the palmar scarring is removed, patients can go home on the day of surgery.
Of course, before going home, we will check the stability of vital parameters (blood pressure, pulse, respiration, body temperature).
We recommend that your operated hand is bandaged until the first follow-up examination.
We will provide you with a prescription for painkillers, but it is better to get them earlier than on the day of the operation if you have a well-established and effective painkiller.
You will receive your final report, which will tell you what to look out for in the post-operative period and when you will have your follow-up examination.
Step 5
A few tips and ideas for the home
After the operation, the hand should be rested, the fingers can only move minimally, and you should not yet touch objects. Do not let the operated hand hang down; keep it elevated.
A few days after the operation, the surgeon removes the silicone drainage tubes that were inserted during the operation.
8-10 days afterwards, after the stitches have been removed, the wound may be exposed to water and the rubber gloves used for washing may be discarded.
Later, we recommend calendula cream skin care and scar management may include ultrasound or laser therapy, depending on your surgeon’s recommendation.
Patients can usually do hard physical work (e.g. woodcutting) 2-3 months after the operation without complaints.
Dupuytren's contracture - Frequently asked questions
No. The specialist treating you decides who can be treated conservatively and who needs surgery, based on the clinical examination, the time of onset of the disease and the patient's comorbidities.
Not really. The first 5-7 days may be moderate pain, but this can be well controlled with painkillers. People usually know their pain tolerance: ask their doctor for a weak, medium or strong painkiller. After a few days the pain is minimal or gone. This can be misleading and may prompt a lot of activity, but it is important to respect the rest period.
On the day of surgery. We usually recommend that anaesthetised patients stay 1 night in hospital if they live a long distance away.
The first check-up is usually scheduled after 2-3 days, because the blood drainage tube (drain) must be removed from the surgical site. Later, the suture removal is scheduled 7-14 days after the operation (depending on the patient's age and co-morbidities).
It depends on what. Until the stitches are removed, we recommend that you keep your hands off the ground, keep them tied up and move your fingers only minimally. After the stitches are removed, you can hold lighter objects and use your computer keyboard.
If I have had an operation on my left hand or if the car has an automatic gearbox: 2-3 days after the operation. If I had surgery on my right hand and the car has a conventional manual gearbox, for safety reasons I recommend that you do not drive for 2-3 days after the stitches are removed (sudden gear changes can be painful and therefore risky).
It depends on your job:
- If you mean oral guidance: from the next day, of course.
- It also depends on which hand I operated on.
- If you use the dominant hand (the one you write with) then depending on the amount of writing required (e.g. 10-20 signatures) you can sign after stitching.
- Using a computer from about the time of stitching is complaint-free.
- You can do light physical work after 4-8 weeks.
- Heavy physical work is possible after about 12 weeks.
Both have advantages and disadvantages. These should be discussed with your doctor. My recommendation is that the patient should have the operation under general anaesthesia or local anaesthesia:
- From the age of
- By gender
- From muscle mass
- From weight
- Depends on your ability to tolerate pain
Of course, we will consult with the patient and take their wishes into account as much as possible.
In the hand, blood vessels, nerves, tendons and muscles are located very close to each other, so damage to them is not excluded. This is most common when the disease has been present for a long time and the shrinkage causes the aforementioned formations to change their position. Even with the most carefully planned surgery, complications can occur which may lead to further treatment and surgery.
Depending on the location and extent of any damage, it may occur:
- Temporary or permanent loss of sensation/feeling around skin incisions, caused by the cutting of skin nerves, postoperative bleeding.
- Swelling of the hand even when the hand is raised.
- Sometimes wound healing disturbances (mainly caused by under-preparation of the skin, which is a well-curable lesion and does not lead to dysfunction).
- Very rarely, deep-seated infections (abscess, arthritis).
- Swollen, painful scarring.
- In exceptional cases, soft tissues may become painful, local circulation is impaired (leading to local cold sensations), with atrophy of bone and muscle tissue, and reduced joint mobility. This lesion (Sudeck's reflex dystrophy) requires urgent follow-up treatment.
Unfortunately, yes. 5 years after various treatments, the disease has a 40-60-80% probability of recurrence.
Unfortunately, yes, in fact it is more common. Many patients have it on both hands at the same time, just with different severity. It is possible to operate on the 2 hands a few months apart.
Yes. More specifically, scarring of connective tissue similar to Dupuytren's contracture can occur in other parts of the body. On the upper limb, on the back of the hand, above the middle joint of the long fingers, these are called Garrod knots or knuckle knots. On the lower limb, scarring of the plantar fascia is called Ledderhose syndrome. Scarring thickening of the connective tissue in the penis is Peyronie's disease.
In this case, the initial scarred knots develop into a string, which bends the finger/fingers, causing permanent loss of mobility in the fingers and functional difficulties (difficulty driving, dressing, gripping, pocketing) in addition to aesthetic disturbance. In long-standing cases, the joints are also damaged, which cannot be completely eliminated even by surgery.
No. In addition to extended surgery, there is a procedure under local anaesthesia to resolve palmar fasciitis, which gives a similar result to injections. The procedure involves administering an anaesthetic to the skin of the palm and then using a thick, strong needle to cut away the tight bundles, improving the range of motion of the fingers.
Unfortunately, we cannot give such a guarantee. Despite the best treatment, Dupuytren's contracture recurs with a high frequency, but the time of recurrence cannot be predicted. At the first sign of recurrence, it is worth consulting your doctor, as your quality of life may improve significantly with surgery.
If you have any questions about Dupuytren’s contracture, please contact us!
Call us
Online booking
