Hip Replacement Without Muscle Cutting
Whether you have just started to explore the possibilities prior to hip replacement or your general practitioner recommended this page, you found the right place. We help you to receive thorough information on muscle-sparing hip replacement (push-aside method).
The very first hip replacement operation was implemented by Sir John Charnley in the 1960s in England. Since then the majority of joint implant surgeries involve hip joint. This type of operation went under significant development since the 1960s: shape and material of prostheses as well as the method of replacement has improved constantly. Recently the so-called muscle-sparing surgery is proved to be one of the best solutions. Due to the nature of this approach the operation leaves muscles of the hip intact resulting the decrease of post-surgical pain and the acceleration of patient rehabilitation.
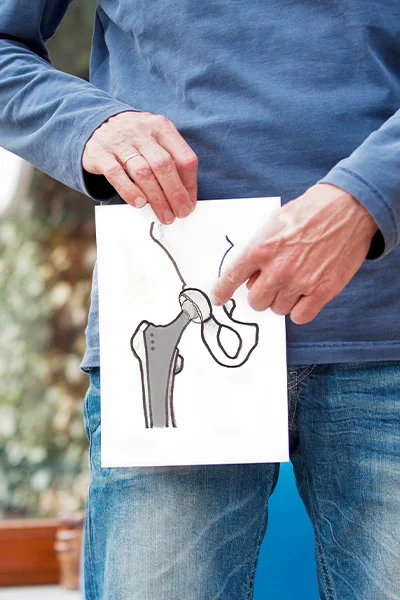
Anatomy of the Hip
Hip joint is like a big spherical joint. The head of the thigh bone (femur), i.e. the rounded and cartilage-covered end of the bone serves as the ball. The part of the hip bone accommodating this ball is called a socket or, using the scientific term, acetabulum. It is a cavity of the pelvic bone also covered with cartilage.
Hip joint is like a big spherical joint. The head of the thigh bone (femur), i.e. the rounded and cartilage-covered end of the bone serves as the ball. The part of the hip bone accommodating this ball is called a socket or, using the scientific term, acetabulum. It is a cavity of the pelvic bone also covered with cartilage. These cartilage surfaces easily slide on each other when the hip joint is healthy. Synovial fluid provides lubrication for smooth movement. This liquid also nurtures joint cartilages.
Strong ligamental connections around the hip joint ensure its stability. Small proximal arteries connect to the femur neck facilitating circulation in the head of the thigh bone. In case of circulatory disorders tissues die in the head section that leads to early joint wear.
Most Common Causes of Hip Joint Pain
Chronic pain in hip joint can most frequently induced by arthrosis, i.e. the wear of cartilage surface within the joint. This can be caused mainly by primary arthrosis, rheumatoid arthritis or secondary arthrosis developed as a consequence of an injury.
- Wear-induced joint inflammation:
It’s also called as degenerative joint disease, osteoarthritis or wear-and-tear arthritis. It is the single most common source of hip joint pain. It generally occurs over 50 years of age. Joint surfaces become worn and fragmented. Instead of cartilages bones connect directly to each other resulting intensive pain and narrowed movement. Sometimes there is no explanation for this kind of disease. - Rheumatoid arthritis:
Its other name is polyarticular inflammation. This autoimmune disease causes an inflammation that is responsible for the damage of the cartilage. As a consequence, the joint becomes swollen and painful. In case the inflammation persists cartilage gradually deteriorates and bone deformities appear around the joint. - Post-traumatic joint wear:
Following a femoral neck or pelvic (acetabulum) fracture caused by an accident the cartilage of the joint is damaged. In the course of time this cartilage induces an inflammation, followed by the pain and reduced movement of the joint. - Avascular femoral head necrosis:
It is also called osteonecrosis. Circulatory disorder takes place in the proximal arteries supplying femoral head. This part of the bone dies and collapses causing sudden great pain in the hip. In the worst case people may become unable to walk. - Congenital hip deformity (hip dysplasia):
Due to an inborn hip dislocation or undeveloped hip joint the cover of femoral head significantly decreases. It can be accompanied by the pathological alteration of the ideal angle between the femoral neck and the femur, since it intensifies joint wear, too. Although some of these lesions can be treated in childhood, they likely lead to early hip joint wear.
The Surgical Process
During the operation the damaged femoral head is removed.
The cartilage found in the acetabulum is also removed and shaped by using a series of ball-cutters. A hemisphere-shaped metal socket is put in this place in which either a hardened plastic liner is inserted or a plastic socket is glued using bone cement.
A metal stem is implanted into the medullary cavity of the thigh bone. This can be done without glue – in this case the stem is wedged into the bone. The other solution requires bone cement with which the metal stem is glued to the bone.
A metal or ceramic ball is put in the stem. This ball moves in the plastic component of the socket as a substitute for the original joint.
Patient Eligibility
During the examination your treating physician interrogates you and records data of antecedence related to the disease. The doctor checks the movement of both hip joints and reviews all x-ray, CT or MR images made earlier. If necessary, he can prescribe other imaging examinations. Your attention is called to the importance of body weight, since it can significantly influence the durability of the prosthesis following the surgery. In due cases pre-surgery physiotherapy, cycling or swimming is advised. Based on the judgement of the physician analgesic treatment or cartilage-regenerating food supplement is recommended. Provided that you have already received treatments, the wear of your hip joint is at an advanced stage and no further improvement can be expected by applying conservative treatment, surgery is suggested.
Giving you thorough information is the task of the physician. Based on this you shall make the decision about the operation. Earlier unsuccessful treatments, constant chronic pain, distress felt overnight as well as considerably restricted movement range can largely influence this decision.
BMM Physicians Performing Hip Replacement Surgery

Dr. Gergely Holnapy PhD
Orthopaedic traumatologist, assistant professor
Dr. Gergely Holnapy PhD
Orthopaedic traumatologist, assistant professor
“I intend to listen to my patients with maximal expertise and maximal politeness.”
Although he treats adults as well, he mainly has children patients here in our practice. He observed that in many cases parents are uncertain about judging certain development changes. They would like me, as a professional, to decide whether the change in question is normal or pathological. Fortunately, the majority of these cases indicate normal development processes.
During his university studies Dr. Gergely Holnapy was interested in manual therapies. He was a fourth-year student when he attended on a rectorial competition in which he wrote about a treatment used in paediatric orthopaedics. The journey that started there and led to the present was full of conferences and professional scholarships in Hungary, Europe and overseas. “I was attending Semmelweis University when gates opened offering the possibility of travel, not only as tourists, but also for professional reasons. In case you want to get a wider and fuller picture about your field of expertise it is necessary to learn about other trends and treatments so that you can establish your own methods. That is why I consider this experience gained both here and abroad important.”
Dr. Holnapy likes cycling and skiing in his spare time. “Sports are a part of my life, although it is not easy to make some time for recreation. However, listening to our patients is really important in this hectic world.”

Dr. Szabolcs Gáspár
Orthopaedic traumatologist, BMS head of department
Dr. Szabolcs Gáspár
Orthopaedic traumatologist, BMS head of department
Dr. Szabolcs Gáspár mainly deals with hip and knee joint disorders. He conducts prosthetic surgeries and treats patients suffering musculoskeletal injuries. He is a professional soldier and university lecturer who regularly participates in Hungarian and international conferences in order to exchange knowledge and experience. His love for medical profession dates back to his childhood.
“Even in kindergarten I wanted to be a traumatologist, as my grandma has told me. When I went to medical university I put that idea of mine temporarily aside, since this branch seemed to be the most difficult. I decided to be orthopaedic surgeon instead. As fate would have it, I became a specialist in both fields and I have never regretted it. They complement each other extremely well within our profession. I like to operate and there is nothing better than doing what you really like to do.”
He considers education as an integral part of his medical career. “I like to teach. It is our future. If we can prepare and educate the next generation than there will always be people able to treat patients. We must show medical students how can good, expert and interesting medical care be given.” Dr. Szabolcs Gáspár put all these in practice alongside the following principles:
“The patient is always right. We must ask adequate questions to reveal their symptoms. In this way they can help us making the diagnosis.” According to Dr. Gáspár it is also indispensable to give explanation to patients about their diseases, the causes and the possible treatments. “It happens from time to time that patients arrive to my office with complete clinical picture. Several examinations have already been implemented, but they still do not know and understand the roots of the problem. Here we have time for everything. Patients fully aware of their conditions are patients recovering much faster and easier.”

Dr. Zoltán Bejek PhD
Associate Professor of Orthopedics
Dr. Zoltán Bejek PhD
Orthopaedic head physician
I was raised in a really close-knit family where I learnt how important the power of love and mutual respect were. My mother taught me the value of generous love and my mechanical engineer father endeared mechanics to me. From early childhood I was interested in how everything worked. In elementary school I decided to become a physician, so I was consciously preparing for that since then.
Me and my family spent three years in a distant corner of the world: Cuba. There I could discover how different people could be. I also realised that in some parts of the world solidarity is a key tool for surviving. I started my university studies there and I finished them back in Budapest.
My love for mechanics has led me to a field where biomechanics played important role: orthopaedics. I was a fourth-year student when I started to carry out scientific researches in the Department of Orthopaedics where I started to work in 1997.
From the beginning I worked in units specialised on endoprosthetics, so I was able to learn all the tricks and finesse of it. Currently I am the head of our unit of endoprosthetics. Previously I also worked in spinal and foot surgery units as well.
My profile includes large joint replacements, revision surgeries, arthroscopic surgeries, plastic repair of ligaments and foot operations.
Complete Description of Hip Replacement Surgery Including Preparations and Rehabilitation
Your health is the most important issue for us. Our goal is to efficiently implement the surgery. We now provide you with a list of some fundamental factors that contribute to the success of the operation and reduce the possibility of complications.
Step 1
Be Healthy Before the Operation!
Blood sugar level
You shall complete a blood glucose test during the preparational phase. In case you are diabetic, please, measure your blood sugar level regularly during the weeks prior to the operation. Adequate glycaemic control significantly reduces the risk of wound infection. We carry out a blood sugar test right before the surgery. In case the value is above 6.7 mmol/l the operation is probably postponed.
Smoking
We ask you not to smoke in the last month before the surgery. Smoking deteriorates microcirculation that can lead to wound healing issues. It is in your own interest to quit smoking in this period. Following the operation you are not allowed to smoke for at least 24 hours.
Overweight
Excess weight has harmful effects on your health. We perform hip replacement only for patients with a BMI (Body Mass Index) not exceeding 35. In case your BMI is above this value we can provide help for losing weight.
Eating
Good nutrition is of key importance. Eat a lot of fresh and colourful fruits and vegetables as well as sufficient amount of protein (meat, egg and fish). Reduce the consumption of sugar and carbohydrates (e.g. white flour, pasta, sweet treats, soda pops etc.). Balanced diet contributes to wound healing and regeneration. Please make sure you drink enough water.
Skin
It is also important to have healthy skin. Wounds, abrasions and scratched areas increase the risk of wound infection. Wound in the surgical site results the postponement of the operation.
Oral and dental hygiene
You shall check your teeth with a dentist before the surgery. A bad tooth can act as foci and lead to complications, thus it must be treated prior to the operation.
Plan Your Surgery Ahead: Things to Before and After
Plan Your Surgery Ahead: Things to Before and After
Prepare for the surgery. It is useful having a “Helper”.
This Helper can be a close friend or a relative. They will escort you for the pre-surgery examinations and transport you to the hospital in the day of the operation. They also regularly visit you and take you home in the day of your discharge. They give a helping hand in your everyday tasks at home and pick up your prescribed medication in the pharmacy.
The Helper supports and assists you during the weeks of recovery.
The presence of the Helper facilitates your successful preparation for the operation as well as your post-surgery rehabilitation. With their support you can soon join the group of healthy people living without pain.
Step 2
The First Phase: The Last Visit in the Doctor’s Office
In case you and your physician both opt for surgery preparations shall start.
You shall choose your Helper who should preferably escort you for the last visit.
Acquiring the x-ray and other scan images that are necessary during the planning phase. X-ray is also taken in the hospital before the surgery based on which your operating physician establishes the surgical procedure.
Lab tests and search for foci – these are implemented in the hospital where the surgery takes place as part of the general health check.
Specialist reports – during pre-surgery examinations the anaesthetist determines what kind of previous or recent examination results are necessary to submit.
Step 3
Pre-Surgery Hospital Examinations
A series of examinations are carried out in the hospital in which the surgery is performed. This usually takes about a whole morning up. We would like to pay the surgery cost proportionately. You receive detailed information on all further tasks. Lab tests, bacteriological analyses (nasal and throat mucus), anaesthesiologic and dental examinations are also carried out. Physicians prescribe necessary anticoagulant and analgesic medicine while providing detailed information on their administration.
Step 4
The Day of the Operation
You arrive to the hospital in the morning. Please do not eat anything on that day. You can drink based on the order of the anaesthetist.
Upon arrival a bed is appointed to you. Nurses help you settle and unpack. We ask you to take a shower before the operation.
Your operating physician visits you in your room. They once more explain the surgical process, mark your skin to indicate the side to be operated and discuss post-surgery actions to be taken.
Nurses measure your blood pressure. They also check blood sugar level in case of diabetic patients.
An intravenous cannula is inserted in the forearm through which you receive fluid and antibiotics.
You can choose to sleep during the surgery. If you decide so, please indicate it to the anaesthetist.
The surgical team performs the hip replacement.
Following the operation you are transported back to your hospital room where your blood pressure, heart rate and oxygen saturation is monitored.
If everything is all right you can drink some liquid and later, according to the nurses’ instructions solid food can be consumed, too.
Your operating physician visits you and summarises the events of the surgery.
Nurses check your condition several times during the day. They help you eating your meal. In case you feel really well you can try to get up with help and take a few steps by using medical aid.
Step 5
Hospitalisation and Discharge
Following the surgery you spend three nights in hospital. In the first morning, during the round, your wound is examined and covered with waterproof bandage so that you can take a shower. You get up with the assistance of a physiotherapist, learn the safe use of elbow crutch and the tricks of leaving the bed and getting back to it. Blood test is taken and, if necessary, blood is given to you. This task is skipped in the majority of the cases, since the surgical site has been treated by painkiller and haemostatic injections at the time of wound closure. If post-surgical pain occurred, nurses would give analgesic IV fluid or pill.
By the day of discharge you are able to move, eat, drink and shower on your own. Time of leaving the hospital is negotiated with you. You can travel by an average car sitting in the front right seat. Your Helper should assist you in getting in and out as well as in turning both of your leg at the same time.
Step 6
At Home
Make exercises, move as much as you can in your home. The side involved in the operation can be trained as well by using medical aids. Do not turn onto your wound when lying in bed. Do not cross your operated limb over the other. When lying on your side put a pillow between your knees.
DO NOT FORGET! Learnt physiotherapy exercises are one of the key factors regarding full recovery. Movement facilitates circulation that has beneficial effect both on your hip and on wound healing.
Frequently Asked Questions
Based on your Body Mass Index (BMI=mass in kgs/height2 in metres) surgeon can recommend you losing some weight. Patients with BMI over 35 can expect longer recovery time and increased risk of complications (infections, wound healing disorders, difficulties in breathing and walking, thrombosis, blood loss and pulmonal embolism).
As any surgery, hip replacement can also have unwanted complications. Statistically speaking the possibility of such consequences is between 0.5 and 1.5 percent globally and in our practice as well. Blood loss, thrombosis, embolism, wound healing disorders, infections, dislocation, bone fracture, uneven limb length, temporary or permanent muscle paralysis and temporary or permanent loss of sensation may occur.
Operating physicians and all members of the surgical team do everything to the best of their knowledge in order to avoid such problems. We kindly ask you to strictly keep all our requests and instructions so as to reduce the possibility of complications.
Patients usually spend three nights in hospital following hip replacement. During this time they learn how to move safely by using medical aids, how to get in and get out of bed and how to complete their cleaning routine.
Even best quality and impeccably inserted prostheses wear as time goes by, since two materials of different hardness move on each other. Usually metal or ceramic head touches the plastic socket. Wear material is inevitably produced that may cause bone resorption around the prosthesis. It occurs in approx. 15 to 20 years. During regular control examinations the surgeon checks the stability of the prosthesis and the wear rate of the system. If necessary, partial or full replacement is offered to the patient.
The wound can be painful following the operation. In order to reduce this pain surgeon infiltrates the wound, the surrounding muscles and the subcutaneous tissue with analgesic and haemostatic injections at the end of the operation. Wound pain is different for each patient. Some do not experience any of it, while others feel it more intensively. In this case nurses administer painkilling medication or IV fluid.
Minimally invasive surgery aims the sparing of anatomical features to keep surrounding tissues intact and to preserve muscular structures. It does not necessarily mean the reduction of incision size in the skin, however it can play a role in this outcome. By using this method post-surgery pain can be decreased and the rehabilitation of patients is accelerated.
The size of incision is determined by the need to access different inner structures. Surgeons always strive to apply the smallest possible cut by which they can successfully perform hip replacement. The actual length of the incision is generally around 10 to 15 cm.
Hip replacement are usually performed under spinal anaesthesia. Patients do not have to sleep during the process, therefore this method burdens the body less. However, if a patient opts for sleeping, because they do not want to hear the noises of the operation, it is possible to sleep – but it is still not a deep anaesthesia. In certain cases, when anaesthetists cannot implement spinal anaesthesia, patients must sleep during the operation. That is why it is important not to eat anything on the day of the surgery.
Patients are able to move by using medical aid in the first six weeks following hip replacement. Regular physiotherapy is indispensable in this period. Furthermore, certain moves and exercises shall be avoided, as determined by the surgeon. At the end of this six-week-long period patients can return to most of their usual means of locomotion and they can cease the use of aid, too. 12 weeks after the operation all restrictions are lifted. By this time total muscular strength and stamina are regained. We still recommend to avoid jumping, jolting and falling in order to preserve the prosthesis in good condition for a long time.
It is really depending on the patient in question. Generally speaking some therapeutic gymnastics is needed prior to hip replacement. Following the operation regular exercising is of key importance. Patients can move by using two elbow crutches and may partially load the operated limb.
A waterproof bandage is applied in the operating room. Patients can get up and learn walking with the help of a physiotherapist. They are able to have a shower the way it was taught to them. The bandage can get in touch with water. Its waterproof nature provides problem-free wound healing.
Patients usually spend the day of the operation in bed. The next morning they can get up and, with the assistance of a physiotherapist, learn how to walk by using medical aids. After that they can get up and have a walk at any time.
In rare cases, if the patient’s vital signs are good and they feel good physically, they are allowed to get up in the day of the surgery, with the help of a physiotherapist.
Six weeks after the surgery, when patients can load their full body weight in the operated limb, driving is also allowed. In case of left-side hip replacement and automatic transmission patients can drive following suture removal (i.e. 8 to 10 days after the operation). Since they do not have to push a pedal with their left leg, the strain is not so strong.
It largely depends on the type of job and working conditions. As for people sitting in an office they can work three weeks after the surgery – provided that they can get to their working place. On the other hand, if their daily work includes standing and intensive physical activity it is recommended to wait three months before starting again.
Jumping and jolting is not recommended as well as locomotion requiring extreme hip movement (e.g. running, ballet or certain types of yoga).
Yes. Metal detectors are usually triggered when people with hip replacement are checked. We suggest informing the security guards about the prosthesis. No written justification is needed, since security services cannot accept that. We recommend cooperation with guards who can check the existence of the prosthesis with a hand-held metal detector.
Yes. According to professional principles we strongly recommend to take prophylactic antibiotics (as a preventive measure) before any dental or other operations. It can reduce the risk of developing septic complications.
Yes. We recommend to take x-rays regularly, i.e. annually or once in every two years, as the operating physician instructed. It is important even if you have absolutely no pain or any other complaint. During these controls surgeon checks the stability and wear level of the prosthesis. Sometimes x-rays indicate wear signs earlier than the first symptoms appear. It is much easier to correct these changes caught in time than replacing the entire prosthesis.
Have you had any further questions regarding hip replacement, please write to us!